Carpal Tunnel Syndrome-2019 Clinical Practice Guidelines for Hand Pain and Sensory Deficits
A leading group of physical therapists gathered over a couple year period to review all the most up to date literature on the conservative treatment of carpal tunnel syndrome (CTS). CTS is defined as having a compression of the median nerve going through the carpal tunnel of the wrist, and reproduces pain, numbness, or weakness in the thumb, index, middle, and half of the ring finger all on the palm side of the hand (Wipperman, 2016). 3.8% of the population experiences carpal tunnel syndrome annually, with the prevalence higher among women than men, most common in 40–60-year-olds, and as expected increases in frequency with an increased presence of the following co-morbidities (Ibrahim et al, 2012):
- Smoking
- Diabetes
- Personal history of carpal tunnel syndrome
- Family history of carpal tunnel syndrome
- Work activities which put frequent force or vibration through the wrist such as typing
CTS can be treated surgically with successful outcomes, but also can be intervened with on a conservative basis, such as with physical therapy. I will summarize the latest evidence on how your physical therapists at Physical Therapy First will use the latest research and evidence to help you recover from your carpal tunnel syndrome, with guidance from the 2019 Clinical Practice guidelines for Carpal Tunnel Syndrome (Erickson et al, 2019).
The evidence to support these recommendations for the diagnosis and treatment of your carpal tunnel syndrome is based on a criterion of strong to very weak or poor evidence. The criteria are described in further detail below:
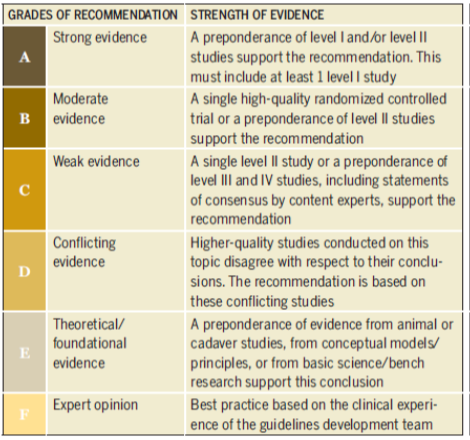
Image from the CTS: CPG, page 6.
Diagnosis
The clinical practice guidelines recommend using the following criterion for proper diagnosis of carpal tunnel syndrome. Your physical therapist at Physical Therapy First will use the most up to date and accurate criterion to provide you with the best information available regarding your diagnosis. The CPG recommends using monofilament testing to assess a person’s response to the feeling of light touch, and the ability to discriminate that touch throughout various parts of your palm and hand. Your physical therapists will also assess the following risk factors which may put you at higher risk of having Carpal Tunnel Syndrome:
- Age >45
- Does shaking your hand relieve your symptoms?
- Do you have loss of sensation in your thumb?
- Is the depth of your wrist >.67% the size of the width of your wrist?
- And upon completing the subjective Boston Carpal Tunnel Questionnaire-Symptom Severity Scale, do you score greater than 1.9? See the BCTQ-SSS, below:
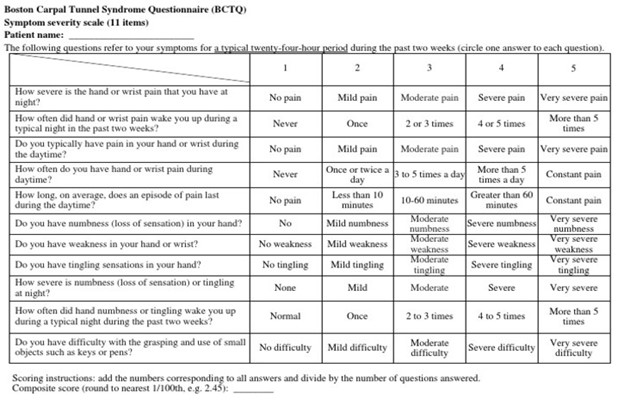
Image courtesy of Levine et al. 1993, the creators of the BCTQ-SSS.
After completion of these 5 risk factors, noting positives on 3 of the 5 leads to an accurate diagnosis of Carpal Tunnel Syndrome. Next, the clinician will perform multiple hands on manual reproductive tests of the wrist (Phalen’s, Tinnel’s, and the Carpal Tunnel Compression Test) to see if compression or palpation of the carpal tunnel reproduces your carpal tunnel symptoms. All of the above diagnostic criteria are rated as ‘A’ or ‘B’, signifying good or very good evidence in support of their performance and accuracy.
Examination
There is either poor evidence or no evidence in support of the following examination criteria to test for Carpal Tunnel Syndrome:
- Lateral Pinch Strength
- Grip strength: Not accurate after surgery, but good examination tool non-surgical
- Conflicting evidence for testing pinch tip strength of the thumb and first and second fingers
- Little or conflicting evidence regarding sensory discrimination, threshold, or vibration testing
Interventions
The following interventions are recommended with strong (A), moderate (B) or weak (C) evidence for Carpal Tunnel Syndrome:
- A neutral positioned wrist splint to be worn at night for short term relief
- Therapeutic exercise including stretching for mild to moderate CTS
- Manual therapy (joint mobilizations, stretching) to the cervical spine and upper extremity for people with mild to moderate CTS
- A trial of electrical stimulation for short term pain relief
- A trial of superficial heat for short term pain relief
Physical Therapists should not use the following treatment interventions due to poor or conflicting evidence for their effectiveness:
- Low level laser
- Iontophoresis
- Thermal or Non-thermal ultrasound
The physical therapists at Physical Therapy First look forward to assisting you in conservative strategies to relieve your carpal tunnel pain and subsequent dysfunction, guided by the best evidence available. Physical Therapy First provides the highest quality care in the Greater Baltimore region with 1 on 1 treatment sessions with your physical therapists for 1 hour. Contact any of our offices (Roland Park, Timonium, Clarksville, or Rosedale today to set up your 1 on 1 consultation with the area’s best physical therapists.
1) Wipperman J, Goerl K. Carpal Tunnel Syndrome: Diagnosis and Management. Am Fam Physician. 2016 Dec 15;94(12):993-999. PMID: 28075090.
2). Ibrahim I, Khan WS, Goddard N, Smitham P. Carpal tunnel syndrome: a review of the recent literature. Open Orthop J. 2012;6:69–76.
3) Erickson M, Lawrence M, Jansen CWS, Coker D, Amadio P, Cleary C. Hand Pain and Sensory Deficits: Carpal Tunnel Syndrome. J Orthop Sports Phys Ther. 2019 May;49(5):CPG1-CPG85. doi: 10.2519/jospt.2019.0301. PMID: 31039690.
