Reviewed by Tyler Tice, PT, DPT, OCS, ATC
Balance is most generally defined as the ability to properly maintain postural control and adapt to various environmental stimuli through the interaction of sensory, motor, and cognitive systems. The three components of balance comprise of the visual system, the vestibular system, and the proprioceptive system. Dysregulation in any of these three systems can result in an increased propensity for falling. It is known that imbalance commonly occurs under dual-task conditions among older adults since cognitive function decreases with aging.
Dual-task training refers to the ability to perform both cognitive tasks and physical activities simultaneously. Due to the fact that both cognitive function and physical function steadily decrease as we age, dual task performance can deteriorate, resulting in falls in older adults when they perform activities of daily living that require maintaining balance. Numerous evidence-based studies have examined the effects of dual-task training on improving balance and reducing fall risks in high-risk older adults, such as individuals with Parkinson’s disease or post-stroke. However, few studies have analyzed the impact of dual-task training on both static and dynamic balance in older adults. Therefore, the aim of this study was to investigate the effects of dual-task training on static balance, dynamic balance, and executive function in older adults with a history of falls.
58 older adults were selected from local senior centers and randomly assigned into either the experimental group or the control group. There were numerous inclusion criteria for these participants: over 65 years of age, experienced falls in the last six months, and those who ambulate independently without any assistive devices. All subjects carried out a 45 min training session, twice a week for 6 weeks, and they only received the training program which was assigned to each group.
In the control group (n=29 participants), subjects conducted the balance training program focusing on body stability, body stability combined with hand manipulation, body transport, and body transport combined with hand manipulation. In the experimental group (n=29 participants), subjects were instructed in dual-task training. These subjects in the experimental group practiced balance tasks while simultaneously conducting cognitive tasks, and were asked to maintain attention to both balance and cognitive tasks at all times. Subjects in both groups completed a total of 12 sessions.
There were numerous outcome measurements utilized in this study. The One Leg Standing Test (OLST) was utilized to assess static balance where a participant places their hands on their hips and raises one leg from the floor with their eyes closed. To assess dynamic balance, the Timed Up and Go (TUG) test was performed where a participant rises from a chair and makes a round trip of 3 meters to sit back in the chair. Lastly, executive function was examined through the Trail-Making Test (TMT-B) .
The findings of this study showed that subjects in the experimental group achieved greater improvements in both static and dynamic balance compared to subjects in the control group. Therefore, the results of this study may indicate that dual-task training might be more effective in improving balance than the more traditionally-utilized functional balance training. Older adults require more attentional resources to maintain balance to compensate for decreases in sensory integration, suggesting cognitive components contribute monumentally to maintaining balance.
Clinical Application:
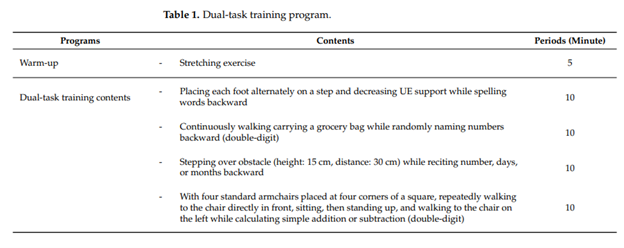
Dual-task training is clinically beneficial to improving static and dynamic balance, as well as executive function in older adults with a history of falls. Additionally, executive function, or the ability to facilitate higher-level cognitive skills, should be considered a major component in balance training for older adults. Below is a graphic of the protocol for the group with dual-task training:
Reference:
Park JH. Is Dual-Task Training Clinically Beneficial to Improve Balance and Executive Function in Community-Dwelling Older Adults with a History of Falls?. Int J Environ Res Public Health. 2022;19(16):10198.
